You’ve tried salicylic acid. You’ve tried benzoyl peroxide. You’ve switched cleansers three times and cut dairy out of your diet. Nothing is working. The tiny, uniform bumps keep appearing across your forehead, chest, or back, and every “acne” product you throw at them seems to make it worse.
Here’s the thing nobody told you: it might not be acne at all. What you’re dealing with could be fungal acne — technically called Malassezia folliculitis — and it requires a completely different approach. Everything in your current routine that’s supposed to help? It might be feeding the problem.
What Fungal Acne Actually Is
Regular acne is caused by bacteria (Cutibacterium acnes) clogging pores. Fungal acne is caused by an overgrowth of Malassezia yeast — a type of fungus that naturally lives on everyone’s skin. When conditions shift in its favor, it multiplies inside hair follicles, causing inflammation that looks a lot like acne but isn’t.
Malassezia feeds on oils, specifically fatty acids with carbon chain lengths of 11-24. That’s important because many skincare products — moisturizers, cleansing oils, even some “acne” treatments — contain exactly those fatty acids. You’re essentially putting yeast food directly on your face.
The yeast triggers an immune response inside the follicle. The result: clusters of small, itchy, uniform bumps that don’t behave like normal breakouts.
How to Tell It Apart From Regular Acne
This distinction matters because the treatments are completely different. If you’re not sure which you have, check our broader acne spot treatment guide for comparison.
Fungal acne looks like:
- Small bumps that are all roughly the same size (1-2mm)
- Clusters rather than individual pimples
- Often itchy — regular acne usually isn’t
- Located on the forehead, chest, back, or along the hairline
- Doesn’t come to a “head” like a normal pimple
- Gets worse in heat, humidity, or after sweating
Regular acne looks like:
- Varied sizes — from tiny blackheads to large cysts
- Mix of different lesion types (whiteheads, blackheads, papules, pustules)
- Usually not itchy
- Often on the lower face, jaw, and chin
- Responds to standard acne treatments within 4-8 weeks
The telltale sign: if your breakouts are uniform, itchy, and don’t respond to traditional acne products after 6-8 weeks of consistent use, fungal acne is very likely.
Why Standard Acne Treatments Make It Worse
This is where most people get trapped in a frustrating cycle.
Antibiotics kill bacteria but don’t touch fungus. Worse, by killing off competing bacteria on the skin, antibiotics can give Malassezia more room to grow. Some people develop fungal acne specifically because they’ve been on oral antibiotics for regular acne.
Heavy moisturizers often contain fatty acids, esters, and oils that feed Malassezia directly. Polysorbates, fatty alcohols (cetyl alcohol, stearyl alcohol), and most plant oils are on the yeast’s menu.
Occlusive products trap heat and moisture against the skin, creating the warm, humid environment Malassezia thrives in.
Oil-based cleansers — not all of them, but many — use oils with carbon chain lengths that feed the yeast. Double cleansing with the wrong oil cleanser can worsen fungal acne significantly.
The Fungal-Safe K-Beauty Routine
The strategy is simple: strip your routine down to products that don’t feed Malassezia, add one antifungal treatment, and wait. Fungal acne responds fast once you stop feeding it — most people see improvement within 1-2 weeks.
Step 1: Fungal-Safe Cleanser
You need a cleanser that removes sweat, sebum, and product residue without leaving behind oils or fatty acid residues that feed the yeast. Low pH is ideal because Malassezia thrives in slightly alkaline environments.
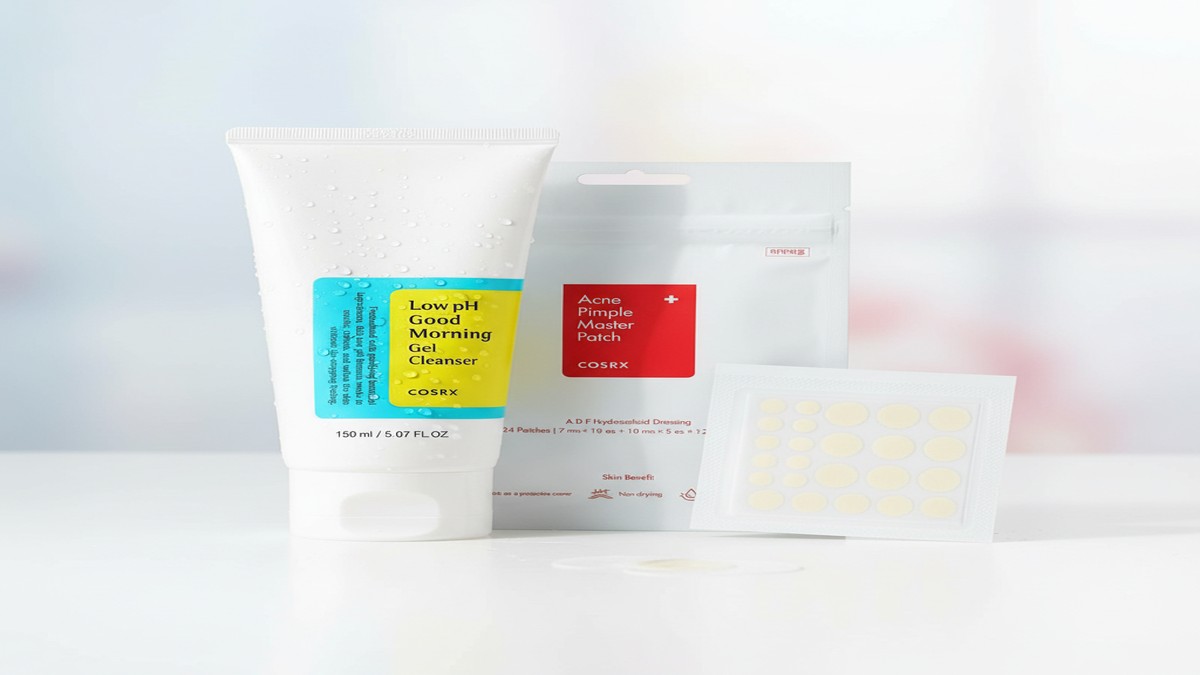
The COSRX Low pH Good Morning Gel Cleanser is one of the safest options. It’s a gel formula (no oils), pH-balanced around 5.0-5.5, and contains tea tree oil which has mild antifungal properties. It cleanses without stripping, and every ingredient is Malassezia-safe.
Shop COSRX Low pH Good Morning Gel Cleanser →
Use it morning and evening. If you wear heavy sunscreen, do a first cleanse with micellar water (fungal-safe) before the gel cleanser.
Step 2: Treatment / Hydration
Your skin still needs hydration, but you need to get it from ingredients Malassezia can’t metabolize. Snail mucin, hyaluronic acid, and glycerin are all safe.
The COSRX Advanced Snail 96 Mucin Power Essence is a workhorse here. It’s 96% snail secretion filtrate, deeply hydrating, helps with healing, and contains nothing Malassezia can feed on. It also helps repair the skin barrier that fungal acne often compromises.
Shop COSRX Snail 96 Mucin Power Essence →
Apply 2-3 pumps to damp skin after cleansing. Let it absorb for 30 seconds before the next step. For more on how to build a proper skincare routine, see our full guide.
Step 3: Antifungal Treatment
This is the step that actually kills the overgrowth. There are two proven approaches:
Ketoconazole cream (2%) — available over the counter in most countries as an antifungal cream. Apply a thin layer to affected areas after cleansing and before moisturizer. Use for 2-4 weeks.
Zinc pyrithione soap or wash — dandruff shampoos containing zinc pyrithione or selenium sulfide are antifungal. Apply to affected areas, leave for 3-5 minutes, rinse off. This sounds strange for a face treatment, but dermatologists have recommended it for decades.
Step 4: Sunscreen
Sunscreen is non-negotiable, but many sunscreens are loaded with fungal-acne triggers — fatty alcohols, esters, and heavy emollients. You need a lightweight, fungal-safe formula.
The PURITO Daily Go-To Sunscreen is a solid choice. It’s lightweight, layers well under makeup, and won’t clog pores or feed yeast. Check our roundup of the best Korean sunscreens for more options, but verify each formula against a Malassezia-safe ingredient checker.
Shop PURITO Daily Go-To Sunscreen →
Step 5: Spot Treatment (As Needed)
For stubborn individual bumps, the COSRX Acne Pimple Master Patch works on fungal acne too. The hydrocolloid material draws out fluid and protects the follicle from further irritation. They’re particularly useful at night when you might unconsciously scratch itchy bumps.
Shop COSRX Pimple Master Patch →
Products to Avoid When You Have Fungal Acne
This list will feel long, and that’s the frustrating part. Many beloved K-beauty products are Malassezia triggers.
Oils to avoid: coconut oil, olive oil, sweet almond oil, argan oil, jojoba oil (controversial — some consider it safe), rosehip oil. Most plant oils with C12-C24 fatty acid chains feed the yeast.
Ingredients to avoid: fatty alcohols (cetyl alcohol, cetearyl alcohol, stearyl alcohol), polysorbate 60 and 80, most esters (isopropyl palmitate, isopropyl myristate), squalane is generally safe but squalene (without the “a”) is not.
Product types to be cautious with: rich sleeping packs, oil-based cleansers, heavy sheet mask essences, emollient lip balms applied near the jawline.
The cheat code: use an online Malassezia-safe ingredient checker. Copy a product’s full ingredient list, paste it in, and it will flag any triggers. Do this before buying anything new.
How to Prevent Recurrence
Fungal acne tends to come back, especially in warm weather or during periods of heavy sweating. Prevention is easier than treatment:
- Shower immediately after exercise. Malassezia thrives on sweat.
- Change out of sweaty clothes. That post-gym errand run in your damp sports bra is an invitation.
- Keep your fungal-safe routine even after skin clears.
- Use a zinc pyrithione wash once a week as maintenance.
- Avoid prolonged antibiotic courses when possible (discuss with your doctor).
- Keep your routine simple and appropriate for your skin type.
Frequently Asked Questions
How quickly does fungal acne clear with the right products?
Most people see significant improvement within 7-14 days of switching to a fungal-safe routine and using an antifungal treatment. The uniform bumps flatten and stop itching within the first week. Complete clearance typically takes 2-4 weeks. If you see no improvement after 3 weeks, revisit every product in your routine — even one trigger ingredient can sustain the overgrowth.
Can I still use acids if I have fungal acne?
Yes, most acids are fungal-safe. Salicylic acid (BHA), glycolic acid (AHA), and azelaic acid all have the green light. In fact, azelaic acid has mild antifungal properties and can help. Just make sure the vehicle (the formula around the acid) doesn’t contain trigger ingredients. Always check the full ingredient list.
Is fungal acne contagious?
No. Malassezia yeast lives on everyone’s skin naturally. Fungal acne happens when conditions favor its overgrowth — heat, humidity, suppressed immune function, antibiotics, or occlusive products. You can’t “catch” it from someone else.
Can I wear makeup over fungal acne?
Yes, but choose your products carefully. Mineral powder foundations and loose setting powders are generally safe. Liquid foundations often contain trigger ingredients — check every formula. Remove makeup thoroughly every evening with a fungal-safe cleanser.
Will fungal acne leave scars?
Fungal acne rarely causes deep scarring the way cystic acne can. However, picking or scratching the bumps (easy to do since they’re itchy) can lead to post-inflammatory hyperpigmentation — dark marks that take weeks to months to fade. Keep your hands off, use pimple patches on spots you’re tempted to touch, and learn about fading dark spots if any marks do appear.
Once the bumps are gone, the next concern is usually the bumpy, clogged surface they leave behind. Our textured skin and clogged pores reset routine is the gentle four-week reset built specifically for that aftermath.